Journal Description
Journal of Cardiovascular Development and Disease
Journal of Cardiovascular Development and Disease
is an international, scientific, peer-reviewed, open access journal on cardiovascular medicine published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, CAPlus / SciFinder, and other databases.
- Journal Rank: CiteScore - Q2 (General Pharmacology, Toxicology and Pharmaceutics)
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 20.3 days after submission; acceptance to publication is undertaken in 2.7 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
2.4 (2022);
5-Year Impact Factor:
3.0 (2022)
Latest Articles
Balloon Valvuloplasty in Congenital Critical Aortic Valve Stenosis in Neonates and Infants: A Rescue Procedure for the Left Ventricle
J. Cardiovasc. Dev. Dis. 2024, 11(5), 156; https://doi.org/10.3390/jcdd11050156 (registering DOI) - 18 May 2024
Abstract
Congenital critical aortic valve stenosis (CAVS) is a life-threatening disease requiring urgent treatment. First-line therapy is still controversial. The aim of our study was (1) to analyze retrospectively the patients of our institution who underwent balloon aortic valvuloplasty (BAV) due to CAVS and
[...] Read more.
Congenital critical aortic valve stenosis (CAVS) is a life-threatening disease requiring urgent treatment. First-line therapy is still controversial. The aim of our study was (1) to analyze retrospectively the patients of our institution who underwent balloon aortic valvuloplasty (BAV) due to CAVS and (2) describe the techniques for improved feasibility of intervention using microcatheters and retrieval loops. Twelve patients underwent 23 BAVs: 1 BAV was performed in 3 patients, 2 BAVs were performed in 7 patients, and 3 BAVs were performed in 2 patients. The peak trans-valvular pressure gradient (Δp) and left ventricular shortening fraction (LVSF) improved significantly in the first two interventions. In the first BAV, Δp decreased from 73.7 ± 34.5 mmHg to 39.8 ± 11.9 mmHg (p = 0.003), and the LVSF improved from 22.3 ± 13.5% to 31.6 ± 10.2% (p = 0.001). In the second BAV, Δp decreased from 73.2 ± 33.3 mmHg to 35.0 ± 20.2 mmHg (p < 0.001), and the LVSF increased from 26.7 ± 9.6% to 33.3 ± 7.4% (p = 0.004). Cardiac surgery during the neonatal period was avoided for all children. The median time to valve surgery was 5.75 years. Few complications occurred, namely mild-to-moderate aortic regurgitation, one remediable air embolism, and one intimal injury to the ascending aorta. We conclude that BAV is a successful emergency treatment for CAVS, resulting in left ventricular relief, clinical stabilization, and a time gain until cardiac surgery.
Full article
(This article belongs to the Special Issue Heart Diseases in Children)
►
Show Figures
Open AccessReview
Untangling the Complex Associations between Socioeconomic and Demographic Characteristics and Prenatal Detection and Outcomes in Congenital Heart Disease
by
Jennifer H. Klein and Mary T. Donofrio
J. Cardiovasc. Dev. Dis. 2024, 11(5), 155; https://doi.org/10.3390/jcdd11050155 (registering DOI) - 18 May 2024
Abstract
Recent literature has established a strong foundation examining the associations between socioeconomic/demographic characteristics and outcomes for congenital heart disease. These associations are found beginning in fetal life and influence rates of prenatal detection, access to timely and appropriate delivery room and neonatal interventions,
[...] Read more.
Recent literature has established a strong foundation examining the associations between socioeconomic/demographic characteristics and outcomes for congenital heart disease. These associations are found beginning in fetal life and influence rates of prenatal detection, access to timely and appropriate delivery room and neonatal interventions, and surgical and other early childhood outcomes. This review takes a broad look at the existing literature and identifies gaps in the current body of research, particularly as it pertains to disparities in the prenatal detection of congenital heart disease within the United States. It also proposes further research and interventions to address these health disparities.
Full article
(This article belongs to the Special Issue Congenital Heart Disease: Risk Factors, Prenatal Diagnosis, and Outcomes)
Open AccessReview
Genetics of Hypertension: From Monogenic Analysis to GETomics
by
Martina Zappa, Michele Golino, Paolo Verdecchia and Fabio Angeli
J. Cardiovasc. Dev. Dis. 2024, 11(5), 154; https://doi.org/10.3390/jcdd11050154 (registering DOI) - 18 May 2024
Abstract
Arterial hypertension is the most frequent cardiovascular risk factor all over the world, and it is one of the leading drivers of the risk of cardiovascular events and death. It is a complex trait influenced by heritable and environmental factors. To date, the
[...] Read more.
Arterial hypertension is the most frequent cardiovascular risk factor all over the world, and it is one of the leading drivers of the risk of cardiovascular events and death. It is a complex trait influenced by heritable and environmental factors. To date, the World Health Organization estimates that 1.28 billion adults aged 30–79 years worldwide have arterial hypertension (defined by European guidelines as office systolic blood pressure ≥ 140 mmHg or office diastolic blood pressure ≥ 90 mmHg), and 7.1 million die from this disease. The molecular genetic basis of primary arterial hypertension is the subject of intense research and has recently yielded remarkable progress. In this review, we will discuss the genetics of arterial hypertension. Recent studies have identified over 900 independent loci associated with blood pressure regulation across the genome. Comprehending these mechanisms not only could shed light on the pathogenesis of the disease but also hold the potential for assessing the risk of developing arterial hypertension in the future. In addition, these findings may pave the way for novel drug development and personalized therapeutic strategies.
Full article
(This article belongs to the Special Issue Advances in the Diagnosis, Treatment, and Risk Stratification of Hypertension)
►▼
Show Figures

Figure 1
Open AccessReview
Rheumatic and Degenerative Mitral Stenosis: From an Iconic Clinical Case to the Literature Review
by
Francesca Napoli, Ciro Vella, Luca Ferri, Marco B. Ancona, Barbara Bellini, Filippo Russo, Eustachio Agricola, Antonio Esposito and Matteo Montorfano
J. Cardiovasc. Dev. Dis. 2024, 11(5), 153; https://doi.org/10.3390/jcdd11050153 - 17 May 2024
Abstract
Mitral stenosis (MS) poses significant challenges in diagnosis and management due to its varied etiologies, such as rheumatic mitral stenosis (RMS) and degenerative mitral stenosis (DMS). While rheumatic fever-induced RMS has declined in prevalence, DMS is rising with aging populations and comorbidities. Starting
[...] Read more.
Mitral stenosis (MS) poses significant challenges in diagnosis and management due to its varied etiologies, such as rheumatic mitral stenosis (RMS) and degenerative mitral stenosis (DMS). While rheumatic fever-induced RMS has declined in prevalence, DMS is rising with aging populations and comorbidities. Starting from a complex clinical case of DMS, the aim of this paper is to review the literature on mitral stenosis by analyzing the available tools and the differences in terms of diagnosis and treatment for rheumatic and degenerative stenosis. Emerging transcatheter techniques, such as transcatheter mitral valve replacement (TMVR) and lithotripsy-facilitated percutaneous mitral commissurotomy (PMC), represent promising alternatives for DMS patients deemed unfit for surgery. In particular, intravascular lithotripsy (IVL) has shown potential in facilitating percutaneous interventions by fracturing calcific deposits and enabling subsequent interventions. However, larger prospective studies are warranted to validate these findings and establish IVL’s role in DMS management. To further enhance this technique, research could focus on investigating the long-term outcomes and durability of mitral lithotripsy, as well as exploring its potential in combination with PMC or TMVR.
Full article
(This article belongs to the Special Issue Innovative Trends in Cardiovascular Medicine and Surgery)
►▼
Show Figures

Figure 1
Open AccessSystematic Review
Cholesteryl Ester Transfer Protein Inhibitors and Cardiovascular Outcomes: A Systematic Review and Meta-Analysis
by
Wajeeh ur Rehman, Merav Yarkoni, Muhammad Abdullah Ilyas, Farwa Athar, Mahnoor Javaid, Muhammad Ehsan, Muhammad Talha Khalid, Ahmed Pasha, Abdelhamid Ben Selma, Alon Yarkoni, Keyoor Patel, Mouhamed Amr Sabouni and Afzal ur Rehman
J. Cardiovasc. Dev. Dis. 2024, 11(5), 152; https://doi.org/10.3390/jcdd11050152 - 16 May 2024
Abstract
Background: Atherosclerosis is a multi-factorial disease, and low-density lipoprotein cholesterol (LDL-C) is a critical risk factor in developing atherosclerotic cardiovascular disease (ASCVD). Cholesteryl-ester transfer-protein (CETP), synthesized by the liver, regulates LDL-C and high-density lipoprotein cholesterol (HDL-C) through the bidirectional transfer of lipids. The
[...] Read more.
Background: Atherosclerosis is a multi-factorial disease, and low-density lipoprotein cholesterol (LDL-C) is a critical risk factor in developing atherosclerotic cardiovascular disease (ASCVD). Cholesteryl-ester transfer-protein (CETP), synthesized by the liver, regulates LDL-C and high-density lipoprotein cholesterol (HDL-C) through the bidirectional transfer of lipids. The novelty of CETP inhibitors (CETPis) has granted new focus towards increasing HDL-C, besides lowering LDL-C strategies. To date, five CETPis that are projected to improve lipid profiles, torcetrapib, dalcetrapib, evacetrapib, anacetrapib, and obicetrapib, have reached late-stage clinical development for ASCVD risk reduction. Early trials failed to reduce atherosclerotic cardiovascular occurrences. Given the advent of some recent large-scale clinical trials (ACCELERATE, HPS3/TIMI55-REVEAL Collaborative Group), conducting a meta-analysis is essential to investigate CETPis’ efficacy. Methods: We conducted a thorough search of randomized controlled trials (RCTs) that commenced between 2003 and 2023; CETPi versus placebo studies with a ≥6-month follow-up and defined outcomes were eligible. Primary outcomes: major adverse cardiovascular events (MACEs), cardiovascular disease (CVD)-related mortality, all-cause mortality. Secondary outcomes: stroke, revascularization, hospitalization due to acute coronary syndrome, myocardial infarction (MI). Results: Nine RCTs revealed that the use of a CETPi significantly reduced CVD-related mortality (RR = 0.89; 95% CI: 0.81–0.98; p = 0.02; I2 = 0%); the same studies also reduced the risk of MI (RR = 0.92; 95% CI: 0.86–0.98; p = 0.01; I2 = 0%), which was primarily attributed to anacetrapib. The use of a CETPi did not reduce the likelihood any other outcomes. Conclusions: Our meta-analysis shows, for the first time, that CETPis are associated with reduced CVD-related mortality and MI.
Full article
(This article belongs to the Section Cardiovascular Clinical Research)
Open AccessArticle
Effects of Water-Based Exercise on Patients Older than 60 Years Undergoing Cardiac Rehabilitation after Coronary Intervention
by
Jus Ksela, Jan Kafol, Danijela Vasic and Borut Jug
J. Cardiovasc. Dev. Dis. 2024, 11(5), 151; https://doi.org/10.3390/jcdd11050151 - 15 May 2024
Abstract
Cardiac rehabilitation (CR) plays a crucial role in managing patients who have undergone coronary intervention (CI) following acute myocardial infarction. While water-based exercise is gaining recognition as an exercise modality in this patient population, its impact on the subgroup of older adults remains
[...] Read more.
Cardiac rehabilitation (CR) plays a crucial role in managing patients who have undergone coronary intervention (CI) following acute myocardial infarction. While water-based exercise is gaining recognition as an exercise modality in this patient population, its impact on the subgroup of older adults remains unexplored. In this post hoc analysis, we investigated the effects of water-based exercise on adults older than 60 years undergoing CR after CI, comparing it to land-based exercise and a control group. In total, 45 patients aged over 60 participated in 14-day exercise programs, featuring two daily 30-min sessions. We assessed exercise capacity (VO2peak), vascular function (flow-mediated vasodilation (FMD)), heart rate variability (HRV), and blood markers (Interleukins 6, 8, and 10, P-Selectin, ICAM, and High-sensitivity CRP) before and after CR. VO2peak in the water-based group improved significantly after CR in comparison with the land-based group: 1.35 kg/mL/min (95% CI [0.20–2.50], p = 0.022). The significant difference between water-based and land-based groups was observed in several HRV parameters: Total power −1129.20 ms2 (95% CI [−1951.92–−306.49], p = 0.008); peak LF 0.04 Hz (95% CI [0.00–0.08], p = 0.036); SD1 −9.02 millisecond (95% CI [−16.86–−1.18], p = 0.025); and SD2 −19.71 ms (95% CI [−35.08–−4.34], p = 0.013). FMD and blood markers did not vary significantly based on the exercise group. These findings suggest that short-term water-based CR may have potential as an alternative to traditional land-based CR, improving VO2peak and cardiorespiratory fitness among adults over 60 years undergoing CR after CI.
Full article
(This article belongs to the Special Issue Exercise and Cardiovascular Disease in Older Adults)
►▼
Show Figures

Figure 1
Open AccessArticle
The Impact of Acute Heart Failure on Frailty Degree and Outcomes in Elderly Patients with Severe Aortic Stenosis and Chronic Heart Failure with Preserved Ejection Fraction
by
Augusto Esposito, Ilenia Foffa, Cecilia Vecoli, Luca Bastiani, Sergio Berti and Annamaria Mazzone
J. Cardiovasc. Dev. Dis. 2024, 11(5), 150; https://doi.org/10.3390/jcdd11050150 - 14 May 2024
Abstract
Frailty degree plays a critical role in the decision-making and outcomes of elderly patients with severe aortic stenosis (AS). Acute heart failure (AHF) results in a severely worse clinical hemodynamic status in this population. This study aimed to evaluate the impact of AHF
[...] Read more.
Frailty degree plays a critical role in the decision-making and outcomes of elderly patients with severe aortic stenosis (AS). Acute heart failure (AHF) results in a severely worse clinical hemodynamic status in this population. This study aimed to evaluate the impact of AHF on frailty degree and outcomes in older patients referred for tailored interventional treatment due to AS. A total of 109 patients (68% female; mean age 83.3 ± 5.4), evaluated by a multidisciplinary path for “frailty-based management” of valve disease, were divided into two groups, one with (AHF+) and one without AHF (AHF-) and preserved ejection fraction (mean value EF: 57.4 ± 8.6). AHF occurred a mean value of 55 days before geriatric, clinical, and surgical assessment. A follow-up for all-cause mortality and readmission was conducted at 20 months. AHF+ patients showed a higher frequency of advanced frailty (53.3% vs. 46.7%, respectively), rehospitalization (35.5% vs. 12.8; p = 0.007), and death (41.9% vs. 12.8%; p < 0.001). In stepwise logistic regression analysis, AHF emerged as an independent risk factor for advanced frailty (OR: 3.8 CI 1.3–10.7; p = 0.01) and hospital readmission (OR: 3.6 CI 1.1–11.6; p = 0.03). In addition, preceding AHF was an independent determinant associated with a higher risk of mortality (HR 2.65; CI 95% 1.04–6.74; p-value 0.04). AHF is independently associated with advanced frailty and poor outcomes in elderly patients with severe AS. So, this population needs careful clinical and geriatric monitoring and the implementation of interventional therapy for AS in the early stages of frailty to avoid the occurrence of AHF and poor outcomes.
Full article
(This article belongs to the Special Issue Prevention and Management of Heart Failure)
►▼
Show Figures

Figure 1
Open AccessCase Report
Multiresistant Kawasaki Disease in a Young Infant with Giant Aneurysms Growing Fast
by
Rosa Amorim-Figueiredo, Ana Pereira Lemos, Tiago Rito, Marta Conde, Maria João Brito and Fátima Pinto
J. Cardiovasc. Dev. Dis. 2024, 11(5), 149; https://doi.org/10.3390/jcdd11050149 - 14 May 2024
Abstract
Background: Kawasaki disease (KD) is a type of vasculitis in which giant coronary artery aneurysms (CAAs) can occur. There are no specific guidelines for managing giant CAAs that develop quickly and are at risk of rupture. Regarding cardiovascular drugs, only beta-blockers are formally
[...] Read more.
Background: Kawasaki disease (KD) is a type of vasculitis in which giant coronary artery aneurysms (CAAs) can occur. There are no specific guidelines for managing giant CAAs that develop quickly and are at risk of rupture. Regarding cardiovascular drugs, only beta-blockers are formally recommended in the acute phase of KD. Case presentation: A 6-month-old male patient with multiresistant Kawasaki disease and giant CAAs that continued to enlarge after controlling systemic inflammation was examined. The patient required three doses of intravenous immunoglobulin, methylprednisolone pulses, and anakinra and infliximab to normalize systemic inflammation. Due to the rapid increment of aneurysms’ dimensions and the risk of rupture, we introduced anticoagulant therapy and propranolol plus captopril, and titration doses were introduced according to a tolerated decrease in heart rate and arterial pressure. CAAs increment stabilized and slowly reduced their dimensions. Conclusions: The authors describe an atypical case of multiresistant KD with giant rapidly increasing CAAs even after controlling systemic inflammation. The introduction of a beta-blocker and an angiotensin-converting enzyme (ACE) inhibitor was demonstrated to be useful for stabilizing giant CAAs growth and reducing the potential risk of rupture.
Full article
(This article belongs to the Special Issue Heart Diseases in Children)
►▼
Show Figures

Figure 1
Open AccessReview
Heart Failure with Mildly Reduced Ejection Fraction—A Phenotype Waiting to Be Explored
by
Anugrah Nair, Lukah Q. Tuan, Natasha Jones-Lewis, Deep Chandh Raja, Jenish Shroff and Rajeev Kumar Pathak
J. Cardiovasc. Dev. Dis. 2024, 11(5), 148; https://doi.org/10.3390/jcdd11050148 - 9 May 2024
Abstract
Heart failure (HF) presents a significant global health challenge recognised by frequent hospitalisation and high mortality rates. The assessment of left ventricular (LV) ejection fraction (EF) plays a crucial role in diagnosing and predicting outcomes in HF, leading to its classification into preserved
[...] Read more.
Heart failure (HF) presents a significant global health challenge recognised by frequent hospitalisation and high mortality rates. The assessment of left ventricular (LV) ejection fraction (EF) plays a crucial role in diagnosing and predicting outcomes in HF, leading to its classification into preserved (HFpEF), reduced (HFrEF), and mildly reduced (HFmrEF) EF. HFmrEF shares features of both HFrEF and HFpEF but also exhibits distinct characteristics. Despite advancements, managing HFmrEF remains challenging due to its diverse presentation. Large-scale studies are needed to identify the predictors of clinical outcomes and treatment responses. Utilising biomarkers for phenotyping holds the potential for discovering new treatment targets. Given the uncertainty surrounding optimal management, individualised approaches are imperative for HFmrEF patients. This chapter examines HFmrEF, discusses the rationale for its re-classification, and elucidates HFmrEF’s key attributes. Furthermore, it provides a comprehensive review of current treatment strategies for HFmrEF patients.
Full article
(This article belongs to the Section Electrophysiology and Cardiovascular Physiology)
►▼
Show Figures

Figure 1
Open AccessCase Report
Management of Ebstein Anomaly in the Current Era: The Story of One Fetus and the Collaboration of Many—A Case Report
by
Ann Kavanaugh-McHugh, Lisa C. Zuckerwise, Stacy A. S. Killen, Emily A. Morris, Rachel T. Sullivan, Mhd Wael Alrifai, David P. Bichell, Melissa Smith-Parrish and Lindsay Freud
J. Cardiovasc. Dev. Dis. 2024, 11(5), 147; https://doi.org/10.3390/jcdd11050147 - 9 May 2024
Abstract
Collaborative multicenter research has significantly increased our understanding of fetal Ebstein anomaly, delineating risk factors for adverse outcomes as well as predictors of postnatal management. These data are incorporated into prenatal care and therapeutic strategies and inform family counseling and delivery planning to
[...] Read more.
Collaborative multicenter research has significantly increased our understanding of fetal Ebstein anomaly, delineating risk factors for adverse outcomes as well as predictors of postnatal management. These data are incorporated into prenatal care and therapeutic strategies and inform family counseling and delivery planning to optimize care. This report details the translation of findings from multicenter studies into multidisciplinary prenatal care for a fetus with Ebstein anomaly, supraventricular tachycardia, and a circular shunt, including transplacental therapy to control arrhythmias and achieve ductal constriction, informed and coordinated delivery room management, and planned univentricular surgical palliation.
Full article
(This article belongs to the Special Issue Congenital Heart Disease: Risk Factors, Prenatal Diagnosis, and Outcomes)
►▼
Show Figures

Figure 1
Open AccessArticle
Role of Lipoprotein Ratios and Remnant Cholesterol in Patients with Myocardial Infarction with Non-Obstructive Coronary Arteries (MINOCA)
by
Vincenzo Sucato, Luca Di Fazio, Cristina Madaudo, Giuseppe Vadalà, Alessandro D’Agostino, Salvatore Evola, Giuseppina Novo, Egle Corrado and Alfredo Ruggero Galassi
J. Cardiovasc. Dev. Dis. 2024, 11(5), 146; https://doi.org/10.3390/jcdd11050146 - 8 May 2024
Abstract
►▼
Show Figures
Background: Myocardial infarction with non-obstructive coronary arteries (MINOCA) is a clinical situation characterized by evidence of acute myocardial infarction (AMI)—according to the Fourth Universal Definition of Myocardial Infarction—with normal or near-normal coronary arteries on angiographic study (stenosis < 50%). This condition is extremely
[...] Read more.
Background: Myocardial infarction with non-obstructive coronary arteries (MINOCA) is a clinical situation characterized by evidence of acute myocardial infarction (AMI)—according to the Fourth Universal Definition of Myocardial Infarction—with normal or near-normal coronary arteries on angiographic study (stenosis < 50%). This condition is extremely variable in etiology, pathogenic mechanisms, clinical manifestations, prognosis and consequently therapeutic approach. Objective: The objective of the study was the evaluation of remnant cholesterol (RC), monocyte/high-density lipoprotein cholesterol ratio (MHR), platelet/lymphocyte ratio (PLR) and various lipoprotein ratios in patients with MINOCA in order to establish their validity as predictors of this event. Materials and Methods: We included 114 patients hospitalized in the Intensive Coronary Care Unit (ICCU) and Hospital Wards of our Hospital Center from 2015 to 2019 who received a diagnosis of MINOCA compared to a control group of 110 patients without previous cardiovascular events. RC was calculated with the following formula: RC = total cholesterol (TC) − HDL-C − LDL-C. MHR was calculated by dividing the monocyte count in peripheral blood by high-density lipoprotein cholesterol (HDL-C) levels; PLR was obtained by dividing platelet count by lymphocyte count. We also calculated various lipoprotein ratios, like total cholesterol/high-density lipoprotein cholesterol (TC/HDL-C), low-density lipoprotein cholesterol/high-density lipoprotein cholesterol (LDL-C/HDL-C), triglycerides/high-density lipoprotein cholesterol (TG/HDL-C), and non-high-density lipoprotein cholesterol/high-density lipoprotein cholesterol (non-HDL-C/HDL-C) ratios. Results: The MINOCA group had higher mean levels of RC (21.3 ± 10.6 vs. 13.2 ± 7.7 mg/dL), MHR (23 ± 0.009 vs. 18.5± 8.3) and PLR (179.8 ± 246.1 vs. 135 ± 64.7) than the control group. Only the mean values of all calculated lipoprotein ratios were lower in MINOCA patients. Statistical significance was achieved only in the RC evaluation. Conclusions: Higher levels of RC and MHR were found in patients with MINOCA. We also observed higher levels of PLR than in the control group. Only various lipoprotein ratios were lower, but this could reflect the extreme heterogeneity underlying the pathogenic mechanisms of MINOCA. In patients who receive a diagnosis of MINOCA with a baseline alteration of the lipid profile and higher levels of cholesterol at admission as well, the evaluation of these parameters could play an important role, providing more detailed information about their cardiometabolic risk.
Full article

Figure 1
Open AccessFeature PaperReview
Semaglutide in Cardiometabolic Diseases: SELECTing the Target Population
by
Francesco Natale, Ettore Luisi, Rosa Franzese, Noemi Mollo, Achille Solimene, Valentina Maria Caso, Andrea Corvino, Paolo Golino and Giovanni Cimmino
J. Cardiovasc. Dev. Dis. 2024, 11(5), 145; https://doi.org/10.3390/jcdd11050145 - 7 May 2024
Abstract
Cardiovascular diseases remain the main cause of death and disability worldwide. Despite the tremendous improvement in pharmacological, minimally invasive and rehabilitative strategies, global deaths due to cardiovascular diseases are still increasing. Additional risk factors have been recently proposed, and thanks to scientific progress,
[...] Read more.
Cardiovascular diseases remain the main cause of death and disability worldwide. Despite the tremendous improvement in pharmacological, minimally invasive and rehabilitative strategies, global deaths due to cardiovascular diseases are still increasing. Additional risk factors have been recently proposed, and thanks to scientific progress, novel drugs for the control of the main risk factors focusing on the cardiometabolic pathways have been identified. Glucagon-like peptide-1 (GLP-1) receptor agonists represent an innovative step in the management of patients affected by type 2 diabetes mellitus. In addition to their significant efficacy on glycemic homeostasis, some members of this class of drugs have indications in the treatment of obesity. Furthermore, accumulated evidence in the literature has finally suggested a protective role in cardiovascular health. The possible role of GLP-1R agonist drugs (GLP-1RAs) on the mechanisms underlying chronic inflammation and the almost ubiquitous distribution of GLP-1 receptors could explain the enormous versatility of these drugs. Semaglutide is a GLP-1RA recently proven to be effective in cardiovascular outcomes. In the present article, we will review the available data on semaglutide in light of the most recent publications to better characterize the target population achieving cardiovascular benefits.
Full article
(This article belongs to the Special Issue Unraveling the Complexities of Cardiometabolic Diseases: Interdisciplinary Insights and Innovative Approaches)
►▼
Show Figures

Figure 1
Open AccessReview
Is Conduction System Pacing a Valuable Alternative to Biventricular Pacing for Cardiac Resynchronization Therapy?
by
Davide Castagno, Francesco Zanon, Gianni Pastore, Gaetano Maria De Ferrari and Lina Marcantoni
J. Cardiovasc. Dev. Dis. 2024, 11(5), 144; https://doi.org/10.3390/jcdd11050144 (registering DOI) - 2 May 2024
Abstract
Cardiac resynchronization therapy (CRT) significantly improves clinical outcomes in patients with ventricular systolic dysfunction and dyssynchrony. Biventricular pacing (BVP) has a class IA recommendation for patients with symptomatic heart failure with reduced ejection fraction (HFrEF) and left bundle branch block (LBBB). However, approximately
[...] Read more.
Cardiac resynchronization therapy (CRT) significantly improves clinical outcomes in patients with ventricular systolic dysfunction and dyssynchrony. Biventricular pacing (BVP) has a class IA recommendation for patients with symptomatic heart failure with reduced ejection fraction (HFrEF) and left bundle branch block (LBBB). However, approximately 30% of patients have a poor therapeutic response and do not achieve real clinical benefit. Pre-implant imaging, together with tailored programming and dedicated device algorithms, have been proposed as possible tools to improve success rate but have shown inconsistent results. Over the last few years, conduction system pacing (CSP) is becoming a real and attractive alternative to standard BVP as it can restore narrow QRS in patients with bundle branch block (BBB) by stimulating and recruiting the cardiac conduction system, thus ensuring true resynchronization. It includes His bundle pacing (HBP) and left bundle branch area pacing (LBBAP). Preliminary data coming from small single-center experiences are very promising and have laid the basis for currently ongoing randomized controlled trials comparing CSP with BVP. The purpose of this review is to delve into the emerging role of CSP as an alternative method of achieving CRT. After framing CSP in a historical perspective, the pathophysiological rationale and available clinical evidence will be examined, and crucial technical aspects will be discussed. Finally, evidence gaps and future perspectives on CSP as a technique of choice to deliver CRT will be summarized.
Full article
(This article belongs to the Special Issue New Pacing Techniques and Non-invasive Methods That May Improve Response and Patient Selection to Cardiac Resynchronization Therapy)
►▼
Show Figures

Figure 1
Open AccessArticle
Association between Abdominal Aortic Calcification and Coronary Heart Disease in Essential Hypertension: A Cross-Sectional Study from the 2013–2014 National Health and Nutrition Examination Survey
by
Lan He, Xu Li, E Shen and Yong-Ming He
J. Cardiovasc. Dev. Dis. 2024, 11(5), 143; https://doi.org/10.3390/jcdd11050143 - 2 May 2024
Abstract
►▼
Show Figures
Background: This study aimed to investigate the association between abdominal aortic calcification (AAC) and coronary heart disease (CHD) in essential hypertension (EH). Methods: This study included patients diagnosed with EH during the 2013–2014 NHANES survey cycle. The study cohort was categorized into the
[...] Read more.
Background: This study aimed to investigate the association between abdominal aortic calcification (AAC) and coronary heart disease (CHD) in essential hypertension (EH). Methods: This study included patients diagnosed with EH during the 2013–2014 NHANES survey cycle. The study cohort was categorized into the following four groups based on their AAC-24 score: no AAC (0); mild AAC (1–4); moderate AAC (5–15); and severe AAC (16–24). Logistic regression models were used to assess the association between AAC and CHD. Restricted cubic spline curves (RCS) were used to explore possible nonlinear relationships between AAC and CHD. Results: The prevalence of CHD was found to be higher in the moderate AAC and severe AAC groups than in the group without AAC (40.1% versus 30.9%, 47.7% versus 30.9%). On a continuous scale, the fully adjusted model showed a 7% increase in the risk of CHD prevalence per score increase in AAC [OR (95% CI) = 1.07 (1.03–1.11)]. On a categorical scale, the fully adjusted model showed the risk of CHD prevalence in EH patients with moderate AAC and severe AAC was 2.06 (95%CI, 1.23–3.45) and 2.18 (1.09–5.25) times higher than that in patients without AAC, respectively. The RCS curve suggested a dose-response linear relationship between AAC and CHD. Conclusion: These findings highlight that in patients with EH, a higher severity of AAC is associated with a higher risk of CHD prevalence.
Full article
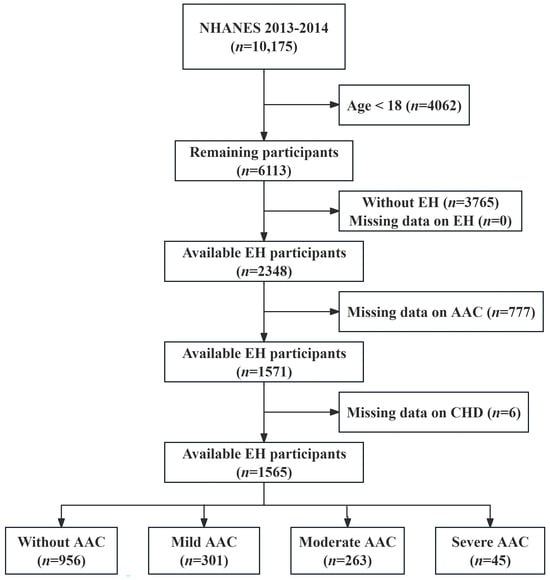
Figure 1
Open AccessArticle
Serum Biomarkers and Their Association with Myocardial Function and Exercise Capacity in Cardiac Transthyretin Amyloidosis
by
Luis Nieto-Roca, Andrea Camblor Blasco, Ana Devesa, Sandra Gómez-Talavera, Jorge Balaguer-Germán, Jairo Lumpuy-Castillo, Ana María Pello, Luis Martínez Dhier, Gregoria Lapeña, Lucía Llanos Jiménez, Óscar Lorenzo, José Tuñón, Borja Ibáñez and Álvaro Aceña
J. Cardiovasc. Dev. Dis. 2024, 11(5), 142; https://doi.org/10.3390/jcdd11050142 - 30 Apr 2024
Abstract
Background: Transthyretin cardiac amyloidosis (ATTR amyloidosis) is a frequent etiology of heart failure. Inflammation and mineral metabolism are associated with myocardial dysfunction and clinical performance. Cardiac global longitudinal strain (GLS) allows function assessment and is associated with prognosis. Our aim was to describe
[...] Read more.
Background: Transthyretin cardiac amyloidosis (ATTR amyloidosis) is a frequent etiology of heart failure. Inflammation and mineral metabolism are associated with myocardial dysfunction and clinical performance. Cardiac global longitudinal strain (GLS) allows function assessment and is associated with prognosis. Our aim was to describe possible correlations between GLS, biomarker levels and clinical performance in ATTR amyloidosis. Methods: Thirteen patients with ATTR amyloidosis were included. Clinical characteristics; echocardiographic features, including strain assessment and 6 min walk test (6MWT); and baseline inflammatory, mineral metabolism and cardiovascular biomarker levels were assessed. Results: Of the 13 patients, 46.2% were women, and the mean age was 79 years. TAPSE correlated with NT-ProBNP (r −0.65, p < 0.05) and galectin-3 (r 0.76, p < 0.05); E/E′ ratio correlated with hsCRP (r 0.58, p < 0.05). Left ventricular GLS was associated with NT-ProBNP (r 0.61, p < 0.05) (patients have a better prognosis if the strain value is more negative) and left atrial GLS with NT-ProBNP (r −0.73, p < 0.05) and MCP1 (r 0.55, p < 0.05). Right ventricular GLS was correlated with hsTnI (r 0.62, p < 0.05) and IL6 (r 0.881, p < 0.05). Klotho levels were correlated with 6MWT (r 0.57, p < 0.05). Conclusions: While inflammatory biomarkers were correlated with cardiac function, klotho levels were associated with clinical performance in the population with TTR-CA.
Full article
(This article belongs to the Section Cardiovascular Clinical Research)
Open AccessReview
Development and Clinical Application of Left Ventricular–Arterial Coupling Non-Invasive Assessment Methods
by
Alvaro Gamarra, Pablo Díez-Villanueva, Jorge Salamanca, Rio Aguilar, Patricia Mahía and Fernando Alfonso
J. Cardiovasc. Dev. Dis. 2024, 11(5), 141; https://doi.org/10.3390/jcdd11050141 - 30 Apr 2024
Abstract
The constant and dynamic interaction between ventricular function and arterial afterload, known as ventricular-arterial coupling, is key to understanding cardiovascular pathophysiology. Ventricular–arterial coupling has traditionally been assessed invasively as the ratio of effective arterial elastance over end-systolic elastance (Ea/Ees),
[...] Read more.
The constant and dynamic interaction between ventricular function and arterial afterload, known as ventricular-arterial coupling, is key to understanding cardiovascular pathophysiology. Ventricular–arterial coupling has traditionally been assessed invasively as the ratio of effective arterial elastance over end-systolic elastance (Ea/Ees), calculated from information derived from pressure–volume loops. Over the past few decades, numerous invasive and non-invasive simplified methods to estimate the elastance ratio have been developed and applied in clinical investigation and practice. The echocardiographic assessment of left ventricular Ea/Ees, as proposed by Chen and colleagues, is the most widely used method, but novel echocardiographic approaches for ventricular–arterial evaluation such as left ventricle outflow acceleration, pulse-wave velocity, and the global longitudinal strain or global work index have arisen since the former was first published. Moreover, multimodal imaging or artificial intelligence also seems to be useful in this matter. This review depicts the progressive development of these methods along with their academic and clinical application. The left ventricular–arterial coupling assessment may help both identify patients at risk and tailor specific pharmacological or interventional treatments.
Full article
(This article belongs to the Section Imaging)
►▼
Show Figures

Graphical abstract
Open AccessArticle
Higher LDL-C/HDL-C Ratio Is Associated with Elevated HbA1c and Decreased eGFR Levels and Cardiac Remodeling in Elderly with Hypercholesterolemia
by
Yufeng Li, Gang Li, Jari A. Laukkanen, Linping Wei and Xinrui Chen
J. Cardiovasc. Dev. Dis. 2024, 11(5), 140; https://doi.org/10.3390/jcdd11050140 - 30 Apr 2024
Abstract
Background: This study aims to explore the relationship of the low-density lipoprotein cholesterol (LDL-C)/high-density lipoprotein (HDL-C) ratio with glycated hemoglobin (HbA1c), renal dysfunction, coronary heart disease (CHD) and cardiac structure and function in elderly patients with hypercholesterolemia. Methods: A total of 1129
[...] Read more.
Background: This study aims to explore the relationship of the low-density lipoprotein cholesterol (LDL-C)/high-density lipoprotein (HDL-C) ratio with glycated hemoglobin (HbA1c), renal dysfunction, coronary heart disease (CHD) and cardiac structure and function in elderly patients with hypercholesterolemia. Methods: A total of 1129 hospitalized Chinese elderly (aged ≥ 65 years) with hypercholesterolemia were collected retrospectively. The patients were divided into low (<2.63), moderate (≥2.63 to <3.33) and high (≥3.33) LDL-C/HDL-C ratio groups according to the tertiles of LDL-C/HDL-C. Results: Regression analysis of the LDL-C/HDL-C ratio with metabolic and echocardiographic parameters revealed that a high LDL-C/HDL-C ratio (≥3.33) was associated independently with male gender, elevated HbA1c, decreased estimated glomerular filtration rate (eGFR), prevalent CHD and left ventricular dilatation (all p < 0.05). Conclusions: A high LDL-C/HDL-C ratio was associated with male gender, increased HbA1c, decreased eGFR, CHD and enlarged left ventricle in elderly with hypercholesterolemia.
Full article
(This article belongs to the Section Cardiovascular Clinical Research)
►▼
Show Figures

Figure 1
Open AccessArticle
Association between Plasma Interleukin-27 Levels and Cardiovascular Events in Patients Undergoing Coronary Angiography
by
Emi Saita, Yoshimi Kishimoto, Reiko Ohmori, Kazuo Kondo and Yukihiko Momiyama
J. Cardiovasc. Dev. Dis. 2024, 11(5), 139; https://doi.org/10.3390/jcdd11050139 - 30 Apr 2024
Abstract
►▼
Show Figures
Atherosclerotic disease, including coronary heart disease (CHD), is one of the chronic inflammatory conditions, and an imbalance between pro-inflammatory and anti-inflammatory cytokines plays a role in the process of atherosclerosis. Interleukin (IL)-27, one of the IL-12 family members, is recognized to play a
[...] Read more.
Atherosclerotic disease, including coronary heart disease (CHD), is one of the chronic inflammatory conditions, and an imbalance between pro-inflammatory and anti-inflammatory cytokines plays a role in the process of atherosclerosis. Interleukin (IL)-27, one of the IL-12 family members, is recognized to play a dual role in regulating immune responses with both pro-inflammatory and anti-inflammatory properties. IL-27 is secreted from monocytes, T cells, and endothelial cells, and its expression is upregulated in atherosclerotic plaques. We previously reported that no significant difference was observed in plasma IL-27 levels between patients with stable CHD and those without it. However, the prognostic value of IL-27 levels has not been fully elucidated. We studied the relation of plasma IL-27 levels to cardiovascular events in 402 patients undergoing elective coronary angiography for suspected CHD. We defined cardiovascular events as cardiovascular death, myocardial infarction, unstable angina, stroke, or coronary revascularization. Of the 402 study patients, CHD was present in 209 (52%) patients. Plasma IL-27 levels were not markedly different between patients with CHD and those without it (median 0.23 vs. 0.23 ng/mL). During a follow-up of 7.6 ± 4.5 years, cardiovascular events were observed in 70 patients (17%). In comparison to the 332 patients with no event, the 70 patients who had cardiovascular events showed significantly higher IL-27 levels (median 0.29 vs. 0.22 ng/mL) and more frequently had an IL-27 level of >0.25 ng/mL (59% vs. 40%) (p < 0.01). The Kaplan–Meier analysis demonstrated a lower event-free survival rate in patients with an IL-27 level >0.25 ng/mL than in those with an IL-27 level ≤0.25 ng/mL (p < 0.02). The multivariate Cox proportional hazards regression analysis showed that IL-27 level (>0.25 ng/mL) was a significant predictor for cardiovascular events (hazard ratio: 1.82; 95%CI: 1.13–2.93, p < 0.02), independent of CHD. Thus, high IL-27 levels in plasma were related to an increased risk of further cardiovascular events in patients who underwent elective coronary angiography.
Full article
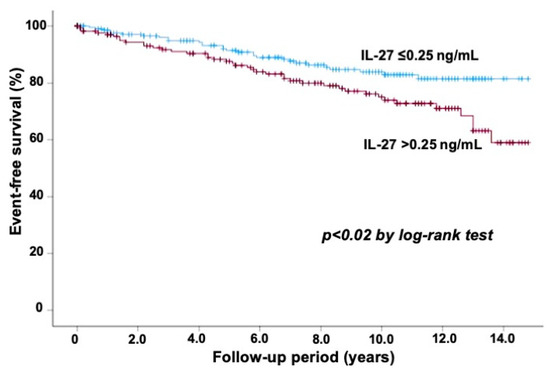
Figure 1
Open AccessArticle
Clinical Features and Patient Outcomes in Infective Endocarditis with Surgical Indication: A Single-Centre Experience
by
Fausto Pizzino, Umberto Paradossi, Giancarlo Trimarchi, Giovanni Benedetti, Federica Marchi, Sara Chiappino, Mattia Conti, Gianluca Di Bella, Michele Murzi, Silvia Di Sibio, Giovanni Concistrè, Giacomo Bianchi and Marco Solinas
J. Cardiovasc. Dev. Dis. 2024, 11(5), 138; https://doi.org/10.3390/jcdd11050138 - 29 Apr 2024
Abstract
Background: Infective endocarditis (IE) is marked by a heightened risk of embolic events (EEs), uncontrolled infection, or heart failure (HF). Methods: Patients with IE and surgical indication were enrolled from October 2015 to December 2018. The primary endpoint consisted of a composite of
[...] Read more.
Background: Infective endocarditis (IE) is marked by a heightened risk of embolic events (EEs), uncontrolled infection, or heart failure (HF). Methods: Patients with IE and surgical indication were enrolled from October 2015 to December 2018. The primary endpoint consisted of a composite of major adverse events (MAEs) including all-cause death, hospitalizations, and IE relapses. The secondary endpoint was all-cause death. Results: A total of 102 patients (66 ± 14 years) were enrolled: 50% with IE on prosthesis, 33% with IE-associated heart failure (IE-aHF), and 38.2% with EEs. IE-aHF and EEs were independently associated with MAEs (HR 1.9, 95% CI 1.1–3.4, p = 0.03 and HR 2.1, 95% CI 1.2–3.6, p = 0.01, respectively) and Kaplan–Meier survival curves confirmed a strong difference in MAE-free survival of patients with EEs and IE-aHF (p < 0.01 for both). IE-aHF (HR 4.3, 95% CI 1.4–13, p < 0.01), CRP at admission (HR 5.6, 95% CI 1.4–22.2, p = 0.01), LVEF (HR 0.9, 95% CI 0.9–1, p < 0.05), abscess (HR 3.5, 95% CI 1.2–10.6, p < 0.05), and prosthetic detachment (HR 4.6, 95% CI 1.5–14.1, p < 0.01) were independently associated with the all-cause death endpoint. Conclusions: IE-aHF and EEs were independently associated with MAEs. IE-aHF was also independently associated with the secondary endpoint.
Full article
(This article belongs to the Section Acquired Cardiovascular Disease)
►▼
Show Figures
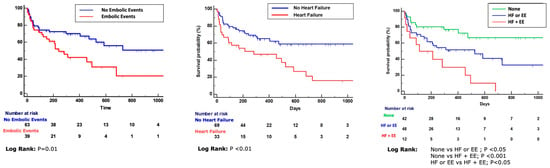
Figure 1
Open AccessArticle
Epicardial Atrial Fat at Cardiac Magnetic Resonance Imaging and AF Recurrence after Transcatheter Ablation
by
Andrea Ballatore, Marco Gatti, Serena Mella, Davide Tore, Henri Xhakupi, Fabio Giorgino, Andrea Saglietto, Ludovica Carmagnola, Edoardo Roagna, Gaetano Maria De Ferrari, Riccardo Faletti and Matteo Anselmino
J. Cardiovasc. Dev. Dis. 2024, 11(5), 137; https://doi.org/10.3390/jcdd11050137 - 28 Apr 2024
Abstract
The relationship between epicardial adipose tissue (EAT) and atrial fibrillation (AF) has gained interest in recent years. The previous literature on the topic presents great heterogeneity, focusing especially on computed tomography imaging. The aim of the present study is to determine whether an
[...] Read more.
The relationship between epicardial adipose tissue (EAT) and atrial fibrillation (AF) has gained interest in recent years. The previous literature on the topic presents great heterogeneity, focusing especially on computed tomography imaging. The aim of the present study is to determine whether an increased volume of left atrial (LA) EAT evaluated at routine pre-procedural cardiac magnetic resonance imaging (MRI) relates to AF recurrences after catheter ablation. A total of 50 patients undergoing AF cryoballoon ablation and pre-procedural cardiac MRI allowing quantification of LA EAT were enrolled. In one patient, the segmentation of LA EAT could not be achieved. After a median follow-up of 16.0 months, AF recurrences occurred in 17 patients (34%). The absolute volume of EAT was not different in patients with and without AF recurrences (10.35 mL vs. 10.29 mL; p-value = 0.963), whereas the volume of EAT indexed on the LA volume (EATi) was lower, albeit non-statistically significant, in patients free from arrhythmias (12.77% vs. 14.06%; p-value = 0.467). The receiver operating characteristic curve testing the ability of LA EATi to predict AF recurrence after catheter ablation showed sub-optimal performance (AUC: 0.588). The finest identified cut-off of LA EATi was 10.65%, achieving a sensitivity of 0.5, a specificity of 0.82, a positive predictive value of 0.59 and a negative predictive value of 0.76. Patients with values of LA EATi lower than 10.65% showed greater survival, free from arrhythmias, than patients with values above this cut-off (84% vs. 48%; p-value = 0.04). In conclusion, EAT volume indexed on the LA volume evaluated at cardiac MRI emerges as a possible independent predictor of arrhythmia recurrence after AF cryoballoon ablation. Nevertheless, prospective studies are needed to confirm this finding and eventually sustain routine EAT evaluation in the management of patients undergoing AF catheter ablation.
Full article
(This article belongs to the Special Issue Modern Approach to Complex Arrhythmias)
►▼
Show Figures
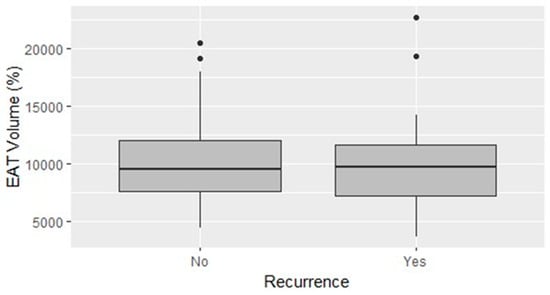
Figure 1

Journal Menu
► ▼ Journal Menu-
- JCDD Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
JCDD, JCM, Medicina, Membranes, ARM
Extracorporeal Membrane Oxygenation (ECMO)
Topic Editors: Patrick Honore, Isabelle MichauxDeadline: 30 November 2024
Topic in
Antioxidants, Biomolecules, JCDD, Metabolites, Neurology International, Pharmaceutics
Tissue-Specific, Disease-Signatured Macrophages in Control of Redox and Antioxidation in Metabolic Diseases
Topic Editors: Xiangwei Xiao, Yingmei Feng, Zhiyong LeiDeadline: 5 July 2025

Conferences
Special Issues
Special Issue in
JCDD
Transcatheter Aortic Valve Implantation (TAVI) II
Guest Editors: Enrico Ferrari, Sergio BertiDeadline: 31 May 2024
Special Issue in
JCDD
Biophysical- and Engineering-Oriented Approaches to Energy-Based Cardiac Ablation Techniques
Guest Editors: Ana González-Suárez, Erik B. Kulstad, Juan J. Pérez, Ramiro Miguel IrastorzaDeadline: 15 June 2024
Special Issue in
JCDD
Peripheral Artery Disease (PAD): Risk Factors, Diagnosis and Treatment
Guest Editor: Zoltán RuzsaDeadline: 30 June 2024
Special Issue in
JCDD
Epidemiology and Long-Term Outcomes in Cardiac Surgery, Thoracic Transplantation, and Interventional Cardiology
Guest Editors: Louise Y. Sun, Matthew William VannemanDeadline: 15 July 2024











